 Last week TDMR obtained a copy of the latest HHS Ombudsman report on complaints about managed care to the agency from Medicaid clients. The report contains a significant section on Dental Managed care.
Last week TDMR obtained a copy of the latest HHS Ombudsman report on complaints about managed care to the agency from Medicaid clients. The report contains a significant section on Dental Managed care.
Medicaid dentists may not get a copy of these reports so we thought we would make them available on our website
After a review of this last report, it is almost unbelievable that out of some 3,428,565 children under the age of 21 enrolled in managed dental care that there were only 43 instances of service that warranted a complaint by a parent or caregiver. Further, only four complaints merited substantiation? It seems that the role of the Ombudsman may not be well-known to parents of Medicaid-eligible children.
It was interesting to find that a main cause of complaint in both quarters of 2021 was access to orthodontic services. The dental managed care section from the latest report is excerpted here but both 2021 reports in PDF form are available below.
Dental Managed Care
The Dental Managed Care program provides all dental services to children on Medicaid under the age of 215. In the second quarter of FY21, OMCAT received 43 complaints, of which 4 (or nine percent) were substantiated. Figure 11 shows a comparison of the top complaint categories for the current quarter and previous fiscal year.
The average monthly enrollment for the Dental Managed Care program in the second quarter of FY21 is 3,428,565.
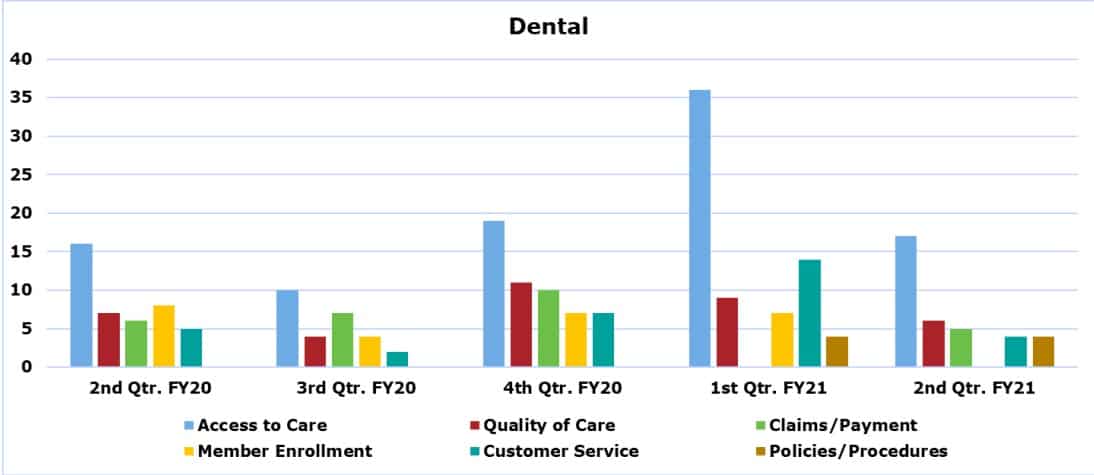
Figure 11 shows complaints related to access to care is the top complaint category beginning in the second quarter of FY20 and into the second quarter of FY21. Data show the top complaint reasons for this category were complaints related to consumers being denied services, access to dental services and issues related to consumers having other insurance.
Complaints related to access to care decreased by 51 percent from the first quarter to the second quarter of FY21. A review of contact reasons shows that there was a decrease in complaints related to accessing dental services. A thorough review of case narratives revealed a decrease in complaints related to consumers having difficulty accessing orthodontic services.
Complaints related to quality of care is the second highest complaint category in the second quarter of FY21. After review of the contact reasons, data show the top complaint reasons for the second quarter of FY21 were complaints of consumers receiving inappropriate or ineffective treatment.
Complaints related to claims and payment is the third highest complaint category in the second quarter of FY21. A review of contact reasons shows the top complaint reasons were complaints of consumers receiving bills for services rendered while active with Medicaid and authorization issues.
Figure 11 also shows that customer service complaints decreased 73 percent from the first quarter to the second quarter of FY21. A review of contact reasons shows there was a decrease in complaints related to staff behavior. A thorough review of case narratives did not reveal a significant trend.

