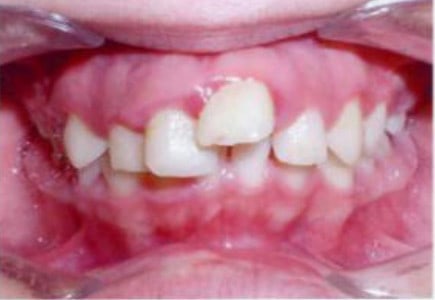
 Earlier this week, TDMR received an email from a mother who had her sons under Medicaid orthodontic treatment back in 2011 and 2012 and is still very upset at the both the state handling of the matter and the lack of concern by MCNA for her sons’ continued treatment. Since 2012, she has been trying without success to get treatment continued for both sons, one with a Class I malocclusion with a crossbite and a deep bite and the other with a Class II malocclusion with a bilateral posterior crossbite and a deep bite.
Earlier this week, TDMR received an email from a mother who had her sons under Medicaid orthodontic treatment back in 2011 and 2012 and is still very upset at the both the state handling of the matter and the lack of concern by MCNA for her sons’ continued treatment. Since 2012, she has been trying without success to get treatment continued for both sons, one with a Class I malocclusion with a crossbite and a deep bite and the other with a Class II malocclusion with a bilateral posterior crossbite and a deep bite.
Approval to tell story
The mother has given us written approval to tell her story. Although this permission includes using her name, for the sake of patient privacy, we are not using it nor the names of providers so her sons cannot be identified.
Medicaid orthodontic treatment from May 2011 until June 2012
The facts of the matter, per the woman, is that both boys had been approved for a full course of Medicaid orthodontic treatment, 26 visits, by the Texas Medicaid and Healthcare Partnership/Xerox back in April 2011. Their treatment started treatment in May 2011 and continued until June 2012 at which time their dental provider went into bankruptcy because their Medicaid payments had been cut off due to “credible allegations of fraud” payment hold. The boys had received eight visits of their 26 visit program.
MCNA took months for initial approvals
Referred to MCNA, the mother was sent by the company to another dentist. But he could not obtain approval from MCNA for continuing the treatment until November, five months later, after numerous calls. However, by the time the appointment rolled around the dentist had moved his practice 26 miles away and she could not make that kind of trip.
During that time, she wrote:
“Over those five months, their teeth began to shift, and their braces had begun to literally come apart; ligatures had rotted off, leading to the wires becoming detached from brackets, and in the case of my younger son, some of the anchor bands had loosened and come off. My younger son was in pain due to a wire that was poking him in the back of his mouth, so I finally took wire cutters to the end of that wire to resolve the pain he was in.”
The whole process had to start again with a new provider who she saw in December. Again the MCNA approval process took months and her sons finally got their braces adjusted in March of 2013.
During the additional three-month wait, she saw that:
“One son’s wires finally came completely off due to ligature disintegration and the other’s wires were almost off. Their teeth had already shifted out of place.”
MCNA had approved one son’s full treatment plan but they only approved four visits for the other son, wrongly concluding he had had 22 previous treatment visits at earlier dental providers. The company could not be persuaded from their position by either the new dentist or the mother who had documentation proving the number of visits.
MCNA changed course and canceled treatment
After the woman had renewed her Medicaid in May, on June 3, 2013, she was told MCNA canceled the one full treatment plan, now determining that the boy had already received full Phase I interceptive orthodontic treatment. The other boy was still allowed the four visits.
The dentist suggested she contact MCNA directly as he could not understand the decision. She wrote the following about her attempt to do that:
“I called Mr. Denis Larry of MCNA twice and left messages. When I received no callback, I emailed him twice a detailed letter about the situation on June 14, 2013. I re-sent the letter six times: June 21, 24, 27, 28 twice, and July 1, 2013, for a total number of eight emails sent. Up until the eighth email was sent, I had not received a response.
“On July 3, 2013, I finally received a message on my answering machine from an MCNA Dental “patient advocate”, Dena Williams. I called her back on July 5th. She told me that she had just received and read my letter; also, she was upset with Mr. Larry for waiting so long to get it to her. She stated that she could not believe what we had been through and that I had a right to be upset and she understood completely. Ms. Williams told me that she had Mr. Larry get the boys’ MCNA Dental records, but she said they couldn’t get [previous bankrupt provider] records because it had been “too long ago.” and they had already been archived. They did have records from [new providers], and those were the only ones they could go by to make a decision. I told her I had the [previous bankrupt provider] records and when [previous bankrupt provider] closed, the boys had received only half their orthodontic treatment. … She told me that [new provider] needed to submit a request for further treatment. Basically, that was the only option she could give me.
“None of this made any sense to me! And I felt as if she was just placating me.”
So since that time, she has been trying to get her sons back into treatment without success. Both boys had their braces removed.
Outraged and hurt by experience
When she wrote us earlier this week, the mother said:
“Hello,
“Why is Texas exempt from following Federal guidelines? I have copied page 13 of “EPSDT-A Guide for States: Coverage in the Medicaid Benefit for Children and Adolescents”.
c. Oral Health and Dental Services
Dental services required in the EPSDT benefit include: Dental care needed for relief of pain, infection, restoration of teeth, and maintenance of dental health (provided at as early an age as necessary); and Emergency, preventive, and therapeutic services for dental disease that, if left untreated, may become acute dental problems or cause irreversible damage to the teeth or supporting structures. In addition, medically necessary oral health and dental services, including those identified during an oral screening or a dental exam, are covered for children. States must provide orthodontic services to EPSDT-eligible children to the extent necessary to prevent disease and promote oral health, and restore oral structures to health and function. Orthodontic services for cosmetic purposes are not covered.
Once a child reaches the age specified by the state in its pediatric dental periodicity schedule, typically age one, a direct dental referral is required. The referral must be for an encounter with a dentist or with another dental professional, such as a dental hygienist, working under the supervision of a dentist. Dental supervision includes the entire range, for example, direct, indirect, general, public health and collaborative practice arrangements.
16 42 C.F.R. § 440.167. 17 Information on CMS efforts working with states to improve access to oral health services for children enrolled in Medicaid and CHIP can be found in CMS, Improving Access to and Utilization of Oral Health Services for Children in Medicaid and CHIP Programs: CMS Oral Health Strategy (April 11, 2011). Approaches states can use to improve the delivery of dental and oral health services to children in Medicaid and CHIP can be found in Keep Kids Smiling: Promoting Oral Health Through the Medicaid Benefit for Children and Adolescents and in Improving Oral Health Care Delivery in Medicaid and CHIP: A Toolkit for States. All of these documents are available at http://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Benefits/DentalCare.html.
18 CMS, State Medicaid Manual § 5124.B.2.b. 19 CMS, State Medicaid Manual § 2700.4 (Form 416 Instructions, Note for Line 12 Data). Dental services are those performed by or under the supervision of a dentist. Oral health services are those performed by other licensed providers not working under the supervision of a dentist, for example, a physician or nurse, or by a dental professional operating without a supervisory relationship to a dentist (e.g., an independent practice dental hygienist). 20 CMS, State Medicaid Manual § 5124.B.2.b 21 42 C.F.R. § 441.56(b)(vi). 22 CMS, State Medicaid Manual § 5123.2.G.
“My family was affected by the Texas Medicaid Orthodontic Witch Hunt of 2012. My sons were approved for the reasons stated on page 13, then denied after we were forced to find another orthodontist for continued treatment.
“Shame on the State of Texas for withholding necessary treatment, and for the hurt it has caused my children!”
Parents with Medicaid-eligible children have “no power or voice”
When we contacted her to find out more about her situation and ask permission to publish her comments, we found she had contacted us late last year. We asked why more parents affected by the situation hadn’t spoken up publicly.
Her answer is enlightening.
“Yes, I was in correspondence with you last year. Thank you again for reading my story and for your attempts to help my situation.
“I still have been unable to get treatment for my sons and have come to the realization that I am powerless over the situation. This is probably the main reason other parents haven’t made complaints or sought help; if a person doesn’t have money, they have no power or voice. I should have accepted that fact earlier, but when my children go through hurt, pain, or injustice, I will try to the best of my ability to get them relief and rectification. What still angers and hurts is to see my boys and others continue to suffer unjustly, as a result of “The Great Texas Dental Medicaid Debacle”. It is wrong!
“I have gained knowledge of how the state of Texas operates Medicaid from my own family’s personal experience as patients, and through sources such as the TDMR website. I also understand the issues and grievances dental providers have gone through dealing with Texas Medicaid. The State of Texas created the mess, a system ruled only by politics, cronyism, money and power. Yet, it has shifted the blame away from themselves. The dentists and the patients are the ones who have been burdened by the fallout of this defective corrupt system. It is shameful, wrong and criminal!
“I really appreciate TDMR’s endeavors for Medicaid reform. You have my permission to use my comments and my name.
“Again thanks.”
State officials ride the gravy train, needy children get the leavings
Two executive staff of the Attorney General can resign, get immediately replaced with new personnel yet continue to draw pay of $28,000 a month between them for absolutely no work for taxpayers. This is all “legal and ethical” per the OAGs office!
The state can waste $20 million on new, untested Medicaid fraud software, the contract given no-bid to friends of Health and Human Services Commission officials. Big hullabaloo, violates state rules but no criminal charges even though that software was dropped like a hot potato and is now replaced by the new IG with 40-year-old software freely available for download by anyone off the HHS-OIG website.
But it is okay for state contractors like MCNA to deny mandated Medicaid orthodontic care to two Texas children that would probably cost less than $3,000 each to complete.
Dentist offers to see what can be done
We are pleased to report that Dr. Chad Evans of the Dental Association for Underserved Children and SmileMagic is looking to see what can be done to help the family.

